The Value of a Pharmacist-Driven Utilization Management Pilot Program
Are you looking for ways to manage the ever-rising costs of specialty drugs and achieving the best return on your investment? Currently, specialty medications account for almost 50% of total US drug expenditure despite only comprising 1-2% of prescription drug claims.1,2 In addition, specialty drug spend is projected to increase, alongside increased FDA approvals for specialty medications. In 2018 alone, 39 out of 59 new drug approvals were for specialty medications. While these agents provide significant improvement in many chronic disease states, specialty medications are associated with serious safety concerns as well as other complications which can further contribute to costs, such as hospitalizations due to adverse effects. Furthermore, it can be difficult to ensure that the goals of therapy are being met with the agent selected due to sparse accessibility of specialty providers.
Until now, self-insured employers have had very few tools to control costs of specialty medications. But The Profero Team has partnered with Valeda Specialty Pharmacy to design a new way to deliver and monitor specialty agents for members, resulting not only in cost-savings, but simultaneously improving outcomes. Historically, pharmacists have been utilized in chronic disease state management programs resulting in improved patient outcomes, patient satisfaction with care, and decreased medical costs.2-9 In the Asheville Project, monitoring by pharmacists resulted in decreased medical costs ($1,200 – $1,872 per patient per year) and decreased number of sick days saving an estimated $18,000 in productivity costs annually, while also improving patient outcomes.3 Currently, pharmacists are being utilized in collaborative practice agreements in order to assist physicians and other healthcare providers in assessing a patient’s medical conditions and medication history in order to make recommendations regarding the most appropriate and most cost-effective therapy.
Our Pharmacist-Driven Utilization Management Program utilizes clinical pharmacists as specialty drug experts, allowing them to take part in a longitudinal drug monitoring program. The goals of this program are seen in the graphic below:
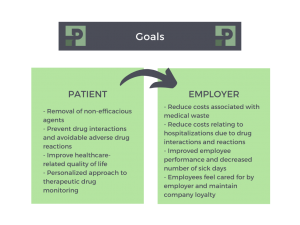
In order to accomplish these goals, each patient has a clinical pharmacist who gathers baseline data such as disease severity, goals of therapy, and the specific agent prescribed by the provider. Following the original data collection, the pharmacist will engage the patient monthly to evaluate adherence, efficacy, drug interactions, and adverse drug effects. The program also monitors the broader impact of specialty management, such as absenteeism, hospital admissions, activity limitations, and additional physician visits and medications prescribed. If a problem is identified, the pharmacist works directly with the patient’s care team to adjust therapy appropriately.
Ultimately, Profero’s pharmacist-directed continuous monitoring program could replace the current system of prior authorizations for specialty medications and provide a greater return on investment. Research has revealed that pharmacists’ engagement in clinical care management results in decreased medical costs of $1800 per patient per year, as well as decreased absenteeism resulting in an $18,000 savings in productivity costs per patient annually. In addition, a March 2018 survey by the American Medical Association revealed that 84% of physicians believed that the burden of prior authorizations (PAs) was “high or extremely high,” with 92% of participants reporting that they believe PAs have a negative impact on patient clinical outcomes.11 Our pilot program would remove the burden of prior authorizations from providers, while allowing pharmacists to provide their expertise in drug therapy monitoring and cost-effective care. Utilizing pharmacists in this regard will identify non-compliant patients, as well as those who are filling high-cost medications that are ineffective or harmful. Instead of a prior authorization completed sporadically, a pharmacist can intervene earlier in therapy in order to maximize outcomes for the patient as well as the employer.
References
- Shu-Ayanji F, Ogurchak J. Expanding the roles of pharmacists: specialty and beyond. Pharmacy Times. Published Online July 13, 2020. Accessed May 4, 2020. Accessed at https://www.pharmacytimes.com/view/expanding-the-roles-of-pharmacists-specialty-and-beyond.
- Zuckerman AD, Carver A, Cooper K, et al. An integrated health-system specialty pharmacy model for coordinating transitions of care: specialty medication challenges and specialty pharmacist opportunities. Pharmacy (Basel). 2019;7(4):163. Doi: 10.3390/pharmacy7040163.
- Cranor CW, Bunting BA, Christensen DB. The Asheville Project: long-term clinical and economic outcomes of a community pharmacy diabetes care program. J Am Pharm Assoc (Wash). 2003;43(2):173-84.
- DiDonato KL, May JR, Lindsey CC. Impact of wellness coaching and monitoring services provided in a community pharmacy. J Am Pharm Assoc (2003). 2013;53(1):14-21. doi: 10.1331/JAPhA.2013.11227.
- Schramm AM, DiDonato KL, May JR, Hartwig DM. Implementation of a financially incentivized weight loss competition into an already established employee wellness program. Innov Pharm. 2014;5(3):Article 170. http://pubs.lib.umn.edu/innovations/vol5/iss3/10
- Theising KM, Fritschle TL, Scholfield AM, Hicks EL, Schymik ML. Implementation and clinical outcomes of an employer-sponsored, pharmacist-provided medication therapy management program. Pharmacotherapy. 2015;35(11):e159-63. doi: 10.1002/phar.1650.
- Janovick DL, Green TR, Bright DR. Assessment of a pharmacist-led comprehensive medication management and wellness program. Inov Pharm. 2015;6(1): Article 192. http://pubs.lib.umn.edu/innovations/vol6/iss1/8
- Liu Y, Guthrie KD, May JR, DiDonato KL. Community pharmacist-provided wellness and monitoring services in an employee wellness program: A four-year summary. Pharmacy (Basel). 2019;7(3):80. doi: 10.3390/pharmacy7030080.
- Yuen J, Bessette H, Gobis B, Kapanen AI, Zed PJ. Participant perceptions of pharmacists and workplace wellness in CAMMPUS. Can Pharm J (Ott). 2020;153(2):80-83. doi: 10.1177/1715163520903744.
- Kibbons AM, Peter M, DeClercq J, et al. Pharmacist interventions to improve specialty medication adherence: study protocol for a randomized controlled trial. Drugs Real World Outcomes. 2020;1-11. doi: 10.1007/s40801-020-00213-8.
- Santa Cruz J. Practice matters: the burden of prior authorizations. Today’s Geriatric Medicine. 2018; 12(1):30. https://www.todaysgeriatricmedicine.com/archive/JF19p30.shtml.